Workup of Microscopic Hematuria
Effective Date: July 29, 2020
This guideline was developed over 5 years ago
Recommendations and Topics
- Scope
- Key Recommendations
- Background
- Definition
- Risk Factors
- Screening for Microscopic Hematuria
- Diagnosis/Investigation
- Follow-up after Negative Workup
- Tests
- Controversy in Care - Should we screen for microscopic hematuria?
- Methodology
- Resources
Scope
This guideline deals with investigation of blood on dipstick urine testing and proven microscopic hematuria in outpatient adults (age 19 and over). Gross hematuria workup is outside of the scope of this guideline. This guideline has been updated in order to limit the unnecessary evaluation (cytology, imaging, & referral) of patients without true microscopic hematuria.
Key Recommendations
- Significant microscopic hematuria is defined as 3 or more RBC/hpf (≥ 3 RBC/hpf) on urine microscopy
- Positive dipstick for hemoglobinuria requires confirmation with urine microscopy testing
- Insignificant microscopic hematuria (0-2 RBC/hpf) does not require further investigation
- Urine microscopy should be collected at the laboratory as the sample must be analysed within 2-3 hours.
- Urine cytology is no longer recommended for routine workup of asymptomatic microscopic hematuria.1
- A single positive urine microscopy (≥ 3 RBC/hpf) should initiate workup as microscopic hematuria is known to be highly intermittent, even in the setting of significant underlying pathology.1
- Significant microscopic hematuria (≥ 3 RBC/hpf) should be investigated with renal function testing (urine albumin-to creatinine ratio (ACR), creatinine/eGFR), blood pressure, imaging and possible referral to urology (as per algorithm below).
- The first line recommended imaging test in most circumstances for the investigation of significant microscopic hematuria is kidney/bladder ultrasound.
- Cystoscopy is recommended for patients with significant microscopic hematuria over the age of 40 or at any age for those with risk factors for urologic malignancy or abnormality on imaging (see Table 1).2,3
- Following a negative workup, urine microscopy, renal function (urine ACR, creatinine/eGFR), blood pressure and urine cytology (if risk factors for urothelial cancer are present) should be followed annually (follow-up can be discontinued after 3 years of negative testing).2
- Indications for repeat investigation:
- Repeat investigation should be undertaken for gross hematuria, new urinary symptoms, or increasing degree of microscopic hematuria, proteinuria, or declining renal function.
- Consideration should be given to repeat investigation if microscopic hematuria persists 3-5 years after initial workup.2
- Screening the general population for microscopic hematuria is not currently recommended.
Background
- The prevalence of microscopic hematuria in the general population ranges from 2.4 to 31.1%.4
- Microscopic hematuria in adults is often an incidental finding but may be associated with urologic malignancy in up to 10% of cases.5
- 33% of male patients ≥ 50 years with hemoglobinuria will ultimately be found to have urologic disease requiring intervention (among whom 25% will have malignancy).6
- Smoking is the most important risk factor for bladder cancer.
- In those over 40 years with microscopic hematuria, the incidence of underlying renal or bladder malignancy increases with age.2
- Bladder cancer is three times more common in men than in women.4
- Microscopic hematuria is also frequently associated with renal parenchymal disease (e.g. glomerular disease).1
- This guideline has been updated to limit the unnecessary evaluation (cytology, referral, imaging) of patients without true microscopic hematuria (≥ 3 RBC/hpf by urine microscopy). Only 14-18% of patients with a positive dipstick have ≥ 3 RBC/hpf by urine microscopy.7
Definition
- Microscopic hematuria is defined as the presence of 3 or more red blood cells (≥ 3 RBC) per high power field (hpf) on a urine microscopy evaluation.1
- Hemoglobinuria on dipstick requires confirmation on urine microscopy before considering investigation.
Risk Factors
Hematuria is the most common sign of bladder cancer. However, the incidence of bladder cancer in patients with microscopic hematuria is low.4
|
Risk Factors for Urothelial Cancer*1,2,4,8 |
|
Demographics • Age > 40 years; risk increases with age2 • Male gender (three times higher in men) • Caucasian ethnicity • Patients with a personal history of bladder cancer Environmental • Smoking, past or present, including exposure to secondhand smoke • Occupational exposure to chemicals or dyes (e.g. benzenes or aromatic amines)** • Exposure to certain drugs (phenacetin, cyclophosphamide) • Overuse of analgesic drugs (phenacetin) • Exposure to pelvic radiation Urologic History • History of gross hematuria • Chronic inflammation of lower urinary tract. (e.g. chronic indwelling foreign body, chronic urinary tract infection, urethral or suprapubic catheter, ureteric stent, bladder stone and chronically infected stone) • History of irritative voiding symptoms • Schistosomiasis haematobium infection (exceedingly rare in North America; endemic to Middle East and Africa) |
*Urothelial includes: renal collecting system, ureter, bladder, prostatic urethra
**Specific occupations at greater risk of bladder cancer: tobacco workers, dye & textile workers, chimney sweeps, nurses, rubber workers, waiters, metal workers, electricians, mechanics, military, public safety workers (police & fire), domestic assistants & cleaners, hairdressers, painters, printers, seafarers, oil & petroleum workers, shoe & leather workers, plumbers, truck drivers, drill press operators, chemical workers and roofers & coal tar workers.4,9,10
Screening for Microscopic Hematuria
- Although there is some evidence to support screening in the general population,6,11 the balance of current evidence and expert opinion is such that screening for microscopic hematuria (with either dipstick or urine microscopy) is not currently recommended. See the Controversies in Care section below.
- There is controversy around whether screening high-risk groups has value. See the Controversies in Care section below.
Diagnosis/Investigation
- If hemoglobinuria is detected on urine dipstick testing (see algorithm below):
- Rule out possible contributing factors such as infection, menstruation, vigorous exercise, trauma to urethra, sexual activity, urological instrumentation, recent prostate exam, or viral illness.
- If these factors are present, repeat the dipstick after resolution of this potentially contributing factor.
- If the dipstick remains positive, confirm with laboratory urine microscopy.
- Further investigation as per the algorithm is warranted if significant microscopic hematuria (≥ 3 RBC/hpf) is present.
- Insignificant microscopic hematuria (≤ 2 RBC/hpf) does not require further investigation.
- Repeat testing may be considered based on clinician discretion and degree of suspicion of occult disease.
- Causes of false positive results for blood on dipstick include: free hemoglobin or myoglobin, menstrual blood, recent exercise and dehydration. Therefore, a positive urine dipstick for blood with a negative urine microscopy (≤ 2 RBC/hpf) can occur.12,13
Important considerations
- Rule out infection prior to further workup/referral for microscopic hematuria.1 Refer to the BC Guideline: Urinary Tract Infection in the Primary Care Setting – Investigation.
- It cannot be assumed that isolated hematuria represents a urinary tract infection.14
- The degree of hematuria does not correlate with the severity of the underlying disease.5
- Anticoagulants, including aspirin, predispose patients to hematuria only in the presence of urinary tract disease. It is recommended that patients on anticoagulants with significant microscopic hematuria (≥ 3 RBC/hpf) be investigated.1
Figure 1. Algorithm: Investigation of Microscopic Hematuria in Adults2
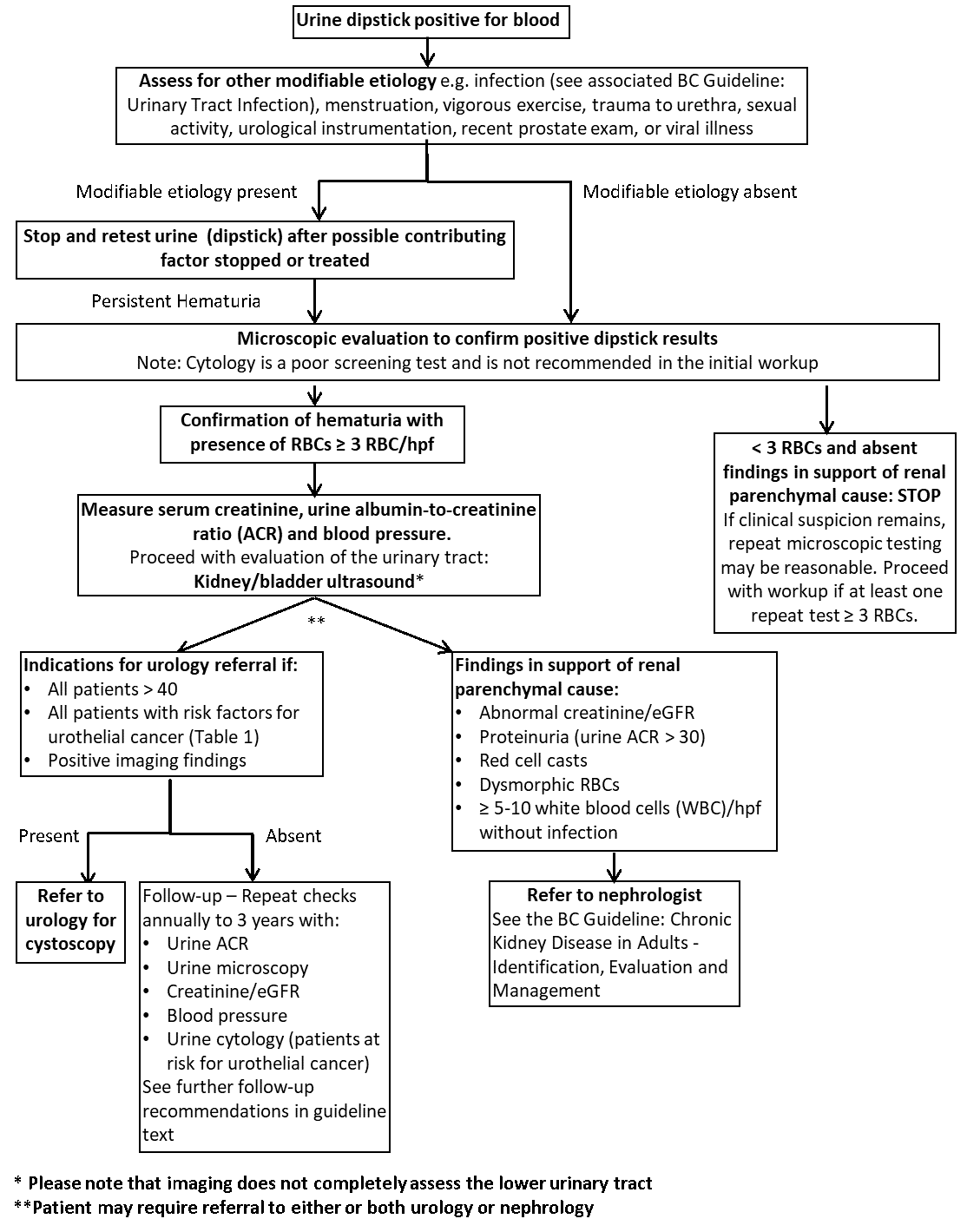
Follow-up after Negative Workup
- No cause will be found for microscopic hematuria in many cases.
- When no specific cause for persistent microscopic hematuria is found, the patient should be followed annually with:2,3
- Urine ACR
- Urine microscopy
- Creatinine/eGFR
- Blood pressure
- Urine cytology (only in patients with risk factors for urothelial cancer)3
- If patients develop gross hematuria, new urinary symptoms, or increasing degree of microscopic hematuria, proteinuria, or declining renal function, reinvestigation as per algorithm should be undertaken.
- If, after initial investigation, the degree of microscopic hematuria persists unchanged on annual follow-up, repeat investigation within 3-5 years should be considered.1
- If three consecutive annual urine microscopies are negative, follow-up testing can be discontinued.1
Tests
1) Urine dipstick vs. urine microscopy
- Unexplained hemoglobinuria on dipstick requires investigation prior to referral.
- Urine dipstick lacks the ability to distinguish red blood cells from myoglobin or hemoglobin.
- A positive dipstick test requires follow-up examination with urine microscopy to confirm the presence of red blood cells.1
- Urine microscopy can distinguish between dysmorphic red cells (renal parenchyma) and isomorphic red cells (urinary collecting system) providing potential insight as to the source of hematuria and direction as to whether a nephrology referral is required in addition to referral to urology.2
- Collection method for urine dipstick and urine microscopy:
- The specimen for urine microscopy must be examined while fresh (within 2-3 hours). This means the patient should go to the lab to give their specimen.
- For any follow-up urine microscopy, sending the patient to the same lab helps with analytical consistency.
- A midstream specimen collected in a clean container without prior cleansing of the genitalia provides a satisfactory sample.
- If the specimen is likely to be contaminated by vaginal discharge or menstrual blood, repeat the sample after resolution.
2) Urine cytology studies:
- Urine cytology studies are no longer recommended for investigation of asymptomatic microscopic hematuria.1
- Urine cytology is still recommended for gross hematuria and symptomatic microscopic hematuria (for which other modifiable etiologies have been ruled out).3
3) Imaging:
- Patients who have evidence of renal parenchymal disease (glomerulopathy) may be appropriately investigated with kidney/bladder ultrasound.
- In most cases, kidney/bladder ultrasound is the preferred initial investigation.
- Kidney/bladder ultrasound and computed tomography intravenous pyelogram (CTIVP) are often used to evaluate the upper urinary tract of patients with microscopic hematuria.
- Traditional intravenous pyelogram (IVP) is still a valid test, however, it is no longer available at many institutions having been supplanted by CTIVP (which provides better detection of renal masses and stones).
- Kidney/bladder ultrasound has comparable sensitivity and specificity, as well as lower morbidity and costs than CTIVP and traditional IVP.
- There is no imaging test (including kidney/bladder ultrasound, CTIVP, and traditional IVP) that completely assesses the lower urinary tract. For this, cystoscopy is required.
- Kidney/bladder ultrasound
Strengths: inexpensive and safest detection of solid masses > 3cm in diameter and hydronephrosis, no ionizing radiation.
Limitations: detection of solid tumors < 3cm in diameter. Kidney bladder ultrasound is preferred over IVP and CT as it has comparable sensitivity and specificity and lower morbidity and costs.
- Computed Tomography Intravenous Pyelogram (CTIVP)
Strengths: detection of renal calculi, small renal and pararenal abscesses, small renal tumors, upper tract urothelial tumors.
Limitations: high cost and limited availability in some areas, equivalent to 2-3 years background radiation exposure.
Note: CTKUB (non contrast CT) and single phase contrast enhanced CT (CT abdomen and pelvis) are not adequate investigations for hematuria.
- Traditional Intravenous Pyelogram (IVP)
Strengths: detecting transitional cell carcinoma of kidney/ureter or renal masses > 3cm in diameter.
Limitations: detecting renal masses < 3cm or lesions of the bladder or urethra, equivalent to 1 year background radiation exposure.
4) Cystoscopy:
- Recommended for:
- all patients > 40 with microscopic hematuria.
- patients of any age with microscopic hematuria and risk factors for urothelial cancer.
- patients of any age with suspicious imaging findings for urologic malignancy.
Controversy in Care - Should we screen for microscopic hematuria?
Screening the general population for microscopic hematuria to detect bladder cancer
- Based on a lack of sufficient evidence, screening the general population for microscopic hematuria is not recommended.
- In 2011, the US Preventative Services Task Force found there was insufficient evidence to assess the benefits and harms of screening for bladder cancer in asymptomatic adults and recently decided there was insufficient new evidence to support an updated review.15
- In 2017, the Société Internationale d’Urologie and International Consultation on Urological Diseases (SIU-ICUD) Joint Consultation did not recommend screening for bladder cancer due to a lack of high-level evidence.4
Screening high-risk groups for microscopic hematuria to detect bladder cancer
- There is conflicting evidence supporting screening high-risk groups for microscopic hematuria.
- In 2017, the SIU-ICUD suggested that targeted screening in those with occupational exposure to potential carcinogens could remove challenges caused by testing the general population.4 The SIU-ICUD considered targeted annual screening with cytology and dipstick of high-risk groups.
- However, a study which included those at high-risk for bladder cancer based on age, smoking status or occupational exposure had a low rate of bladder cancer detection.4,16
Methodology
These guideline recommendations are tailored to support practice in British Columbia and are based on guidance by the American Urological Association1, Canadian Urological Association2 and Canadian Consensus statement3. Where available, key references are provided. In situations where there is a lack of rigorous evidence, we provide best clinical opinion to support decision making and high-quality patient care. The guideline development process included significant engagement and consultation with primary care providers, specialists and key stakeholders, including with Provincial Laboratory Medicine Services. For more information about GPAC guideline development processes, refer to the GPAC handbook available at BCGuidelines.ca.
Resources
Practitioner Resources
- BC Cancer Agency www.bccancer.ca
- Health Info, Bladder
- BC Guideline: Urinary Tract Infection in the Primary Care Setting – Investigation
Patient Resources
- HealthLink BC www.healthlinkbc.ca
Hematuria Diagnostic Code: 599.7
References
1. Davis R, Jones JS, Barocas DA, Castle EP, Lang EK, Leveillee RJ, et al. Diagnosis, Evaluation and Follow-up of Asymptomatic Microhematuria (AMH) in Adults: AUA guideline. [Internet]. American Urological Association 2012 Reviewed 2016. Available from: https://pubmed.ncbi.nlm.nih.gov/23098784/
2. Wollin T, Laroche B, Psooy K. Canadian guidelines for the management of asymptomatic microscopic hematuria in adults. Can Urol Assoc J. 2009 Feb;3(1):77–80.
3. Kassouf W, Aprikian A, Black P, Kulkarni G, Izawa J, Eapen L, et al. Recommendations for the improvement of bladder cancer quality of care in Canada: A consensus document reviewed and endorsed by Bladder Cancer Canada (BCC), Canadian Urologic Oncology Group (CUOG), and Canadian Urological Association (CUA), December 2015. Can Urol Assoc J. 2016;10(1–2):E46–80.
4. Fernández MI, Brausi M, Clark PE, Cookson MS, Grossman HB, Khochikar M, et al. Epidemiology, prevention, screening, diagnosis, and evaluation: update of the ICUD-SIU joint consultation on bladder cancer. World J Urol. 2019 Jan;37(1):3–13.
5. Khadra MH, Pickard RS, Charlton M, Powell PH, Neal DE. A prospective analysis of 1,930 patients with hematuria to evaluate current diagnostic practice. J Urol. 2000 Feb;163(2):524–7.
6. Messing EM, Young TB, Hunt VB, Roecker EB, Vaillancourt AM, Hisgen WJ, et al. Home screening for hematuria: results of a multiclinic study. J Urol. 1992 Aug;148(2 Pt 1):289–92.
7. LifelabsTM. Statistic provided by a Canadian laboratory.
8. Bladder [Internet]. [cited 2019 Nov 14]. Available from: http://www.bccancer.bc.ca/health-info/types-of-cancer/urinary/bladder
9. Cumberbatch MGK, Cox A, Teare D, Catto JWF. Contemporary Occupational Carcinogen Exposure and Bladder Cancer: A Systematic Review and Meta-analysis. JAMA Oncol. 2015 Dec 1;1(9):1282–90.
10. Lange: Symptom to Diagnosis: An Evidence Based Guide, Second Edition [Internet]. [cited 2020 Feb 12]. Available from: http://www.langetextbooks.com/0071808159.php?c=home
11. Messing EM, Madeb R, Young T, Gilchrist KW, Bram L, Greenberg EB, et al. Long-term outcome of hematuria home screening for bladder cancer in men. Cancer. 2006 Nov 1;107(9):2173–9.
12. Mundt LA, Shanahan K. Graff’s Textbook of Routine Urinalysis and Body Fluids. Lippincott Williams & Wilkins; 2010. 352 p.
13. Wein AJ, Kavoussi LR, Novick AC, Partin AW, Peters CA. Campbell-Walsh Urology. Elsevier Health Sciences; 2011. 5689 p.
14. Sharp VJ, Barnes KT, Erickson BA. Assessment of Asymptomatic Microscopic Hematuria in Adults. Am Fam Physician. 2013 Dec 1;88(11):747–54.
15. Final Update Summary: Bladder Cancer in Adults: Screening - US Preventive Services Task Force [Internet]. [cited 2019 Nov 14]. Available from: https://www.uspreventiveservicestaskforce.org/Page/Document/UpdateSummaryFinal/bladder-cancer-in-adults-screening
16. Lotan Y, Elias K, Svatek RS, Bagrodia A, Nuss G, Moran B, et al. Bladder cancer screening in a high risk asymptomatic population using a point of care urine based protein tumor marker. J Urol. 2009 Jul;182(1):52–7; discussion 58.
This draft guideline is based on scientific evidence current as of February 2020.
The draft guideline was developed by the Guidelines and Protocols Advisory Committee in collaboration with Provincial Laboratory Medicine Services.
For more information about how BC Guidelines are developed, refer to the GPAC Handbook available at BCGuidelines.ca: GPAC Handbook.
THE GUIDELINES AND PROTOCOLS ADVISORY COMMITTEE
|
The principles of the Guidelines and Protocols Advisory Committee are to:
Contact Information: Guidelines and Protocols Advisory Committee PO Box 9642 STN PROV GOVT Victoria, BC V8W 9P1 Email: hlth.guidelines@gov.bc.ca Website: www.BCGuidelines.ca
Disclaimer The Clinical Practice Guidelines (the guidelines) have been developed by the guidelines and Protocols Advisory Committee on behalf of the Medical Services Commission. The guidelines are intended to give an understanding of a clinical problem, and outline one or more preferred approaches to the investigation and management of the problem. The guidelines are not intended as a substitute for the advice or professional judgment of a health care professional, nor are they intended to be the only approach to the management of clinical problem. We cannot respond to patients or patient advocates requesting advice on issues related to medical conditions. If you need medical advice, please contact a health care professional. |


 TOP
TOP